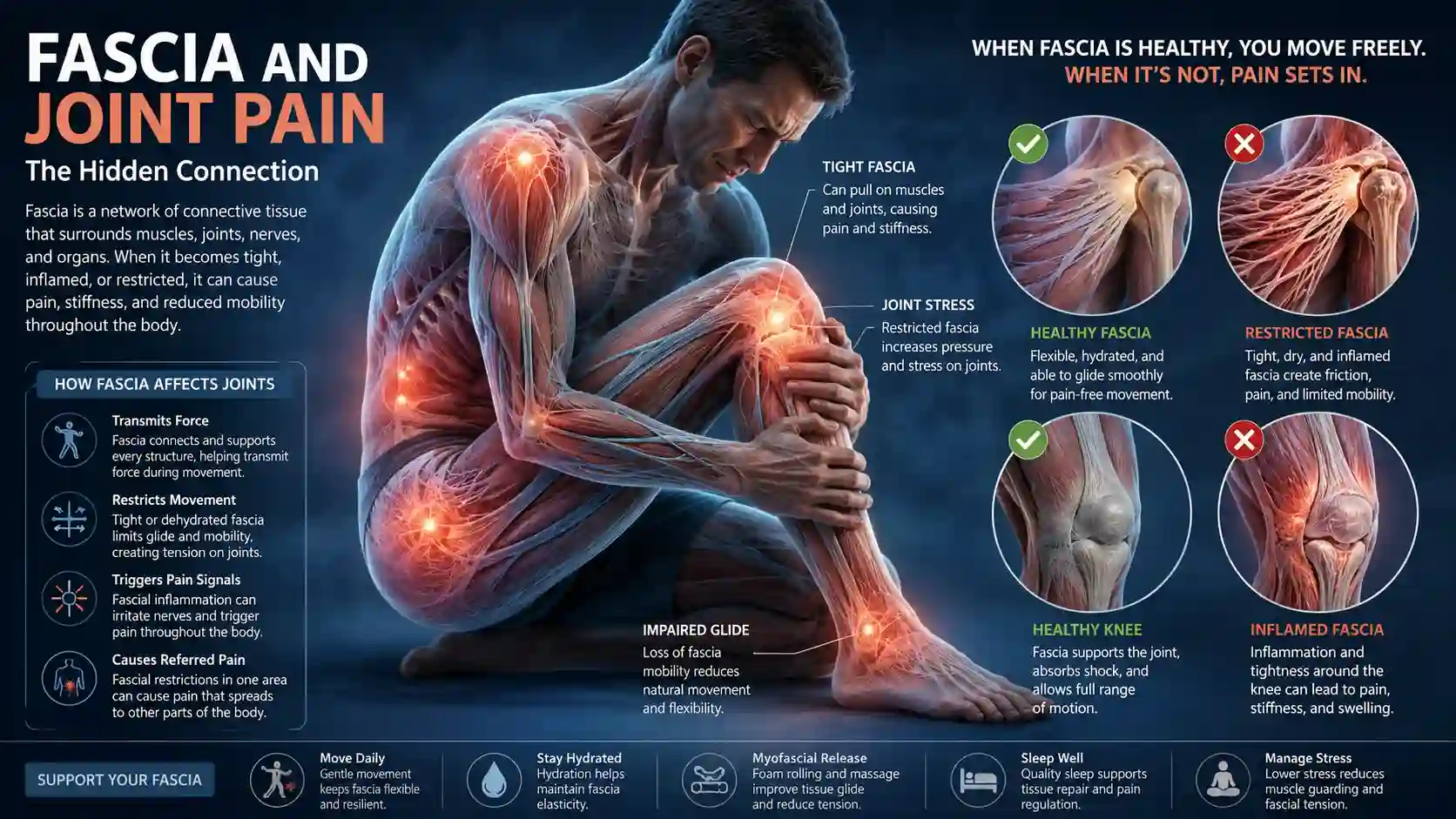
Many people live with aching knees, stiff shoulders, sore hips, or persistent back discomfort without ever receiving a clear explanation. Standard scans sometimes show little damage, blood tests return normal, and treatments aimed only at joints often fail to provide lasting relief. This confusion has pushed researchers and clinicians to look beyond cartilage, bones, and ligaments. One tissue drawing increasing attention is fascia.
The connection between fascia and joint pain is becoming an important topic in rehabilitation medicine, physical therapy, sports science, and chronic pain research. Fascia is a continuous web of connective tissue that surrounds muscles, organs, nerves, blood vessels, and joints. When healthy, it supports smooth movement and stability. When irritated, restricted, or overloaded, it may contribute to pain patterns that feel difficult to explain.
Scientists now believe that fascia contains sensory nerves capable of generating discomfort and altered movement patterns. Research published through institutions such as the National Institutes of Health and scientific journals in musculoskeletal medicine suggests that fascial dysfunction may influence mobility, inflammation, and pain perception. This does not mean fascia explains every chronic condition, but it may help clarify why some people experience body pain even when imaging appears normal.
Understanding fascia provides a broader perspective on how the body functions as one interconnected system rather than isolated parts. It also explains why stress, inactivity, repetitive movement, dehydration, poor posture, and injury can create pain far away from the original problem area.
What is fascia and why does it matter?
Fascia is a thin yet strong connective tissue network found throughout the human body. It wraps around muscles, supports organs, separates tissue layers, and connects structures from head to toe. Unlike muscles or bones, fascia forms a continuous web, meaning tension in one region can affect movement elsewhere.
Researchers once considered fascia little more than packing material. Today, scientists recognize it as an active tissue involved in movement coordination, proprioception, force transmission, and pain signaling. Studies from anatomy and rehabilitation research show that fascia contains nerve endings, blood vessels, and immune cells that respond to physical stress and injury.
Scientists studying chronic pain increasingly associate unexplained stiffness with connective tissue dysfunction affecting normal movement patterns. Researchers continue examining how fascia may contribute to chronic musculoskeletal pain in both active and sedentary populations.
Healthy fascia remains flexible and hydrated. It glides smoothly during movement, allowing muscles and joints to function efficiently. However, inactivity, repetitive strain, trauma, stress, or poor movement habits may reduce this mobility. Over time, restricted tissue can create pulling sensations, stiffness, and discomfort.
This explains why people sometimes experience symptoms that do not match a traditional joint injury. Pain may shift locations, worsen with stress, or appear alongside tightness and reduced flexibility. Fascial restriction can also influence posture and movement mechanics, increasing strain across surrounding tissues.
Scientists studying connective tissue disorders increasingly recognize the role of fascial health in chronic musculoskeletal pain. While more research continues, current evidence strongly supports fascia as an important contributor to movement quality and discomfort patterns.
How fascia affects movement and pain perception
Fascia acts like an internal support network that distributes force throughout the body. During walking, lifting, stretching, or exercise, fascia helps transfer energy between muscles and joints. If this network loses elasticity or hydration, movement efficiency declines.
One reason fascial dysfunction matters is its relationship with the nervous system. Fascia contains sensory receptors that help the brain understand body position and movement. Some studies suggest fascial tissue may contain more pain sensitive nerve endings than muscle tissue itself. This means irritated fascia could contribute directly to chronic soreness or sensitivity.
Researchers studying movement science are increasingly exploring how connective tissue affects chronic pain, especially in patients whose symptoms cannot be explained through standard imaging alone. Poor fascial glide can contribute to broader movement dysfunction throughout the body. In some individuals, persistent soft tissue tension may increase sensitivity during movement.
Restricted fascia may also change how muscles activate. When tissues cannot glide correctly, the body compensates by overusing nearby muscles and joints. This creates uneven stress patterns that may eventually lead to discomfort. Uneven loading patterns can eventually create muscular compensation in nearby regions.
Researchers believe nervous system sensitivity may amplify discomfort associated with fascial irritation. Scientists continue studying how fascia influences pain signaling within the nervous system.
People reporting fascia tightness and pain often describe sensations such as pulling, burning, deep aching, or widespread stiffness. Unlike sharp injury pain, fascial discomfort may feel diffuse and difficult to pinpoint. Symptoms sometimes worsen after long periods of sitting or repetitive activity.
Researchers in sports medicine have also explored how fascial stiffness affects athletic performance and injury recovery. Reduced fascial elasticity may decrease mobility and increase biomechanical stress, potentially contributing to overuse injuries.
This growing understanding challenges the outdated idea that chronic pain always comes from structural joint damage alone. In many cases, soft tissue tension and nervous system sensitivity may play equally important roles.
Common fascia inflammation symptoms people overlook
One reason fascial problems remain misunderstood is that symptoms often mimic other conditions. Many people seek treatment for arthritis, tendon issues, or muscle strain without realizing connective tissue dysfunction may also contribute.
Typical fascia irritation symptoms can include morning stiffness, bodywide tightness, reduced flexibility, tenderness during pressure, and discomfort that moves from one area to another. Some individuals also report fatigue, muscle heaviness, or a sensation of pulling during movement.
Pain linked to fascia often responds differently from acute injuries. It may fluctuate depending on stress levels, sleep quality, hydration, physical activity, or emotional tension. Since fascia interacts closely with the nervous system, psychological stress may increase tissue tension and pain sensitivity.
Many individuals describe unexplained bodywide stiffness that worsens after inactivity. Some patients experience recurring mobility problems even without visible joint damage. Restricted connective tissue may contribute to gradual flexibility loss over time.
Researchers have observed fascial changes in conditions such as chronic low back pain, plantar fasciopathy, fibromyalgia, and myofascial pain syndrome. While these conditions involve multiple factors, connective tissue dysfunction appears to influence symptom severity in some patients.
Another overlooked sign involves reduced range of motion. Tight connective tissue can limit how smoothly muscles slide during movement, causing stiffness without obvious swelling or injury.
Over time, persistent tissue restriction may reduce mobility and alter posture. Persistent tissue restriction may eventually alter posture and walking patterns. This can create additional strain on knees, hips, shoulders, and the spine, further increasing discomfort over time.
Why unexplained joint pain is becoming more common
Modern lifestyles may unintentionally create ideal conditions for fascial dysfunction. Long hours of sitting, limited physical activity, repetitive screen use, stress, and poor recovery habits can all influence connective tissue health.
One of the major unexplained joint pain causes discussed in rehabilitation medicine is movement deprivation. Fascia thrives on regular motion. Gentle stretching, walking, varied movement, and exercise help maintain tissue hydration and flexibility. Without movement, connective tissue may stiffen and lose adaptability.
Modern rehabilitation experts are also investigating why body stiffness happens without injury, particularly among sedentary individuals with long term mobility limitations.
Stress also affects the body physically. Increased muscle guarding during emotional stress can raise tension throughout fascial chains. Over time, this constant low level contraction may contribute to stiffness and pain sensitivity.
Sleep quality plays another major role. Poor sleep interferes with tissue recovery and nervous system regulation, both of which influence chronic pain experiences.
Hydration may matter as well. Fascia contains water rich extracellular material that supports tissue glide. Dehydration may reduce tissue elasticity, although researchers continue studying the exact relationship.
Age related changes can further complicate the issue. Collagen structure naturally changes over time, potentially reducing tissue resilience and increasing stiffness.
Importantly, unexplained pain does not mean imaginary pain. Many chronic pain conditions involve subtle tissue dysfunction and nervous system sensitization that standard imaging may not fully capture.
The scientific link between fascia and joint pain
The relationship between fascia and joint pain has become a major topic in connective tissue research during the last two decades. Studies using ultrasound imaging and microscopic analysis have identified structural changes in fascial tissue among people with chronic musculoskeletal pain.
Researchers have found increased thickness and reduced sliding capacity in thoracolumbar fascia among patients with chronic low back pain. Other studies suggest inflamed fascia may contain elevated inflammatory markers and nerve growth activity associated with pain sensitivity.
Scientists are also investigating how fascial tension spreads mechanical stress across the body. Because fascia forms continuous chains, restriction in one region may influence movement elsewhere. Tightness in the calves, for example, could alter knee mechanics and eventually affect hip or lower back function.
Restricted tissue may gradually interfere with natural movement mechanics during walking and exercise. This interconnected system may explain why some patients fail to improve when treatment targets only the painful joint rather than surrounding tissue patterns.
Another important discovery involves the role of mechanoreceptors within fascia. These receptors respond to pressure, stretch, and movement, helping regulate posture and muscular coordination. Dysfunction in these sensory systems may contribute to chronic pain patterns and movement compensation.
Although research continues evolving, experts increasingly agree that connective tissue health deserves attention in both prevention and rehabilitation programs.
Conditions associated with fascial dysfunction
Several health conditions may involve fascial irritation or restriction alongside other biological factors. One commonly discussed condition linked to fascia is myofascial pain syndrome, where sensitive trigger points create persistent discomfort.
Fibromyalgia research has also explored fascial abnormalities. Some investigators suggest altered connective tissue stiffness and impaired circulation may contribute to widespread tenderness and fatigue.
Athletes frequently experience fascial overload due to repetitive movement patterns. Runners, weightlifters, and office workers alike may develop chronic tension from repetitive stress and poor recovery.
Plantar fasciopathy provides another example. Although commonly linked to the foot alone, modern research views it as part of a larger kinetic chain involving calves, hips, and movement mechanics.
Chronic neck and shoulder discomfort may also involve fascial restriction caused by prolonged screen use and static posture. Many people experiencing fascia tightness and pain notice symptoms worsen after desk work or emotional stress.
Importantly, fascial dysfunction rarely acts alone. Pain usually involves multiple interacting factors including muscle conditioning, sleep, stress, inflammation, posture, and nervous system sensitivity.
Can fascia heal naturally?
Fascial tissue has the ability to adapt and recover, although improvement often requires consistent movement and lifestyle changes rather than quick fixes.
Regular mobility exercises may help maintain tissue glide and hydration. Walking, stretching, yoga, resistance training, and controlled movement practices all encourage healthy tissue loading.
Daily movement and hydration habits may support long term connective tissue health. Adequate sleep and tissue hydration may help maintain connective tissue flexibility.
Foam rolling and myofascial release techniques have gained popularity in rehabilitation and sports medicine. Some studies suggest these approaches may temporarily improve flexibility and reduce discomfort, although long term evidence remains mixed.
Consistent mobility work may support long term movement recovery after periods of inactivity.
Hydration and sleep also support tissue recovery. Since fascia interacts closely with the nervous system, stress management may influence pain sensitivity as well.
Manual therapy approaches such as massage and fascial manipulation are widely used, though researchers continue studying their exact mechanisms. Many clinicians believe these treatments work partly by affecting nervous system regulation and movement awareness rather than physically breaking tissue apart.
People experiencing persistent pain should seek medical evaluation to rule out serious conditions. Fascial dysfunction can overlap with arthritis, autoimmune disease, nerve disorders, and other medical problems requiring proper diagnosis.
Daily habits that may worsen connective tissue stiffness
Modern routines often encourage behaviors linked to reduced mobility and increased discomfort. Sitting for long periods decreases movement variability and may reduce fascial elasticity over time.
Long periods of inactivity often increase feelings of chronic stiffness around major joints.
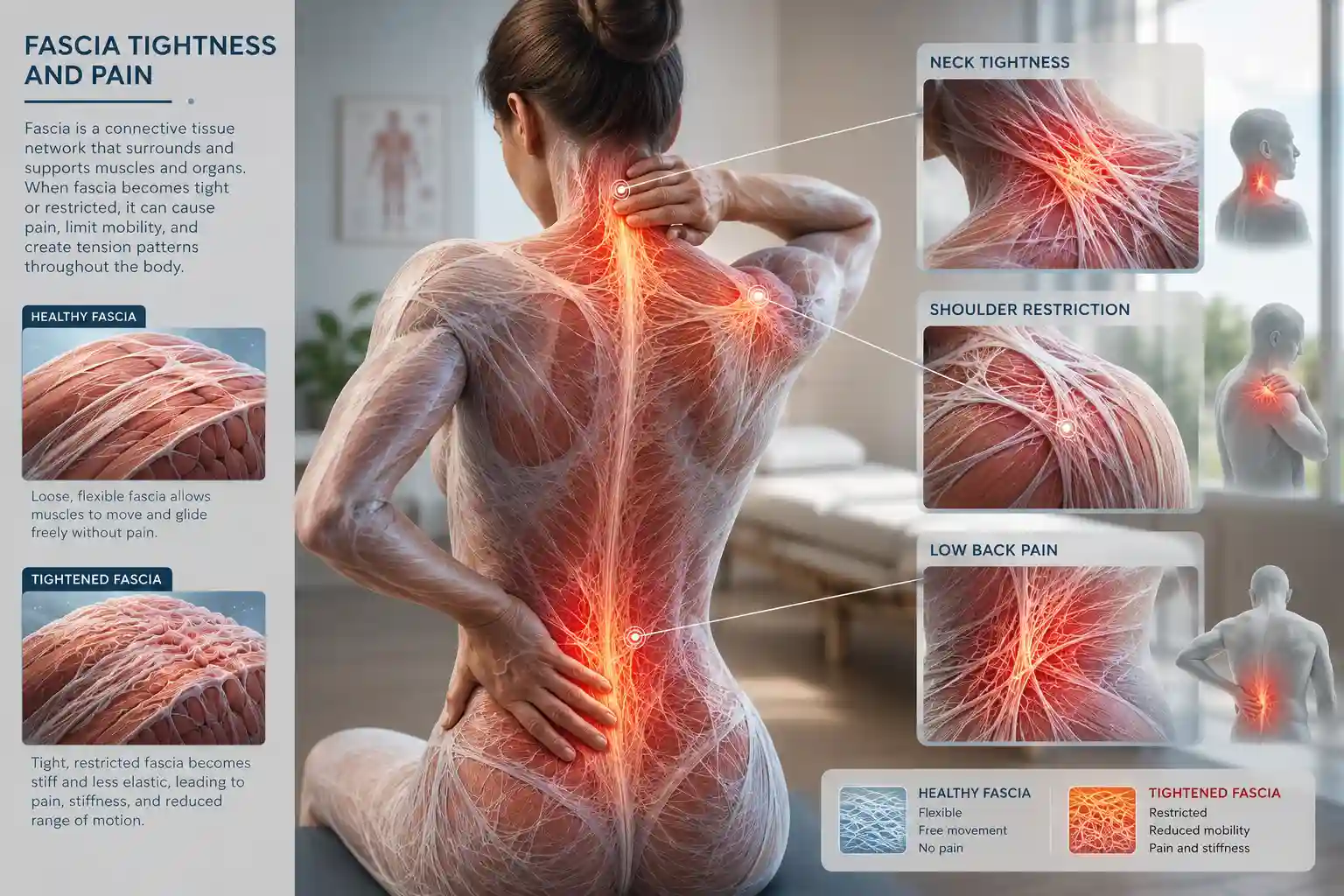
Repetitive movements without recovery can also overload connective tissue. This includes certain workplace tasks, excessive exercise volume, and prolonged screen use.
Chronic psychological stress deserves attention as well. Stress related muscle tension can increase physical stiffness and amplify pain perception.
Poor workstation habits may contribute to posture related pain involving the neck and shoulders.
Poor breathing mechanics may contribute too. Shallow chest breathing can create tension in the neck, shoulders, and rib cage, influencing overall movement patterns.
Ignoring recovery after exercise sometimes worsens tissue irritation. The body requires adequate rest, nutrition, hydration, and sleep to repair connective tissue stress.
People dealing with recurring fascia inflammation symptoms often notice improvements after introducing regular movement breaks, posture variation, stretching, and stress reduction strategies into daily life.
The future of fascia research
Fascia research is still developing, but scientific interest continues growing rapidly. New imaging technologies now allow researchers to observe tissue movement and stiffness more accurately than before.
Scientists are exploring how connective tissue interacts with inflammation, immune signaling, chronic stress, and pain perception. Researchers are also studying the role of fascia in aging, athletic recovery, and rehabilitation outcomes.
Researchers in rehabilitation medicine continue exploring fascia based recovery approaches.
One promising area involves the relationship between connective tissue and the autonomic nervous system. This may help explain why emotional stress influences physical pain so strongly in some individuals.
Another emerging topic examines how sedentary lifestyles affect tissue adaptability. As more people spend extended time sitting, researchers expect chronic movement related pain conditions to rise.
Understanding connective tissue may eventually improve rehabilitation strategies for chronic musculoskeletal disorders and persistent unexplained discomfort.
Conclusion
The growing body of research surrounding fascia and joint pain is changing how experts understand chronic discomfort and movement dysfunction. Rather than viewing the body as isolated parts, modern science increasingly recognizes the importance of interconnected connective tissue systems.
Fascia influences movement, posture, flexibility, and pain signaling throughout the body. When this tissue becomes restricted or irritated, symptoms may appear as stiffness, aching, mobility loss, or persistent discomfort without clear structural damage.
Improved understanding of fascia may help explain persistent chronic body discomfort in many adults.
Also Read: Knee Brace vs Supplement for Knee Pain: Which Works Better Long Term?
Although fascia is not responsible for every chronic pain condition, current evidence suggests it plays a meaningful role in many musculoskeletal complaints. Paying attention to movement quality, stress management, sleep, hydration, and recovery may help support connective tissue health over time.
As research continues evolving, clinicians and researchers will likely develop more effective approaches for identifying and managing chronic discomfort linked to connective tissue dysfunction. For many people struggling with unexplained symptoms, understanding fascia may finally provide missing context behind long standing pain patterns.
Sources and section mapping
- National Institutes of Health
- Harvard Medical School
- Cleveland Clinic
- Journal of Bodywork and Movement Therapies
- Frontiers in Physiology
- National Library of Medicine
FAQs
Can connective tissue restriction affect balance and coordination?
Yes. Fascial tissue contains sensory receptors involved in body awareness and movement coordination. When tissue becomes restricted, the brain may receive altered feedback about posture and positioning. This can affect stability, balance, and movement efficiency during daily activities. Some rehabilitation specialists believe reduced tissue glide contributes to compensation patterns that increase strain on nearby muscles and joints over time.
Why do fascia inflammation symptoms sometimes feel worse during stress?
Stress activates the nervous system and often increases unconscious muscle tension throughout the body. Since connective tissue closely interacts with muscles and nerves, prolonged stress may heighten pain sensitivity and stiffness. Researchers studying chronic pain have found that emotional tension can amplify physical symptoms even without additional tissue injury.
Are unexplained joint pain causes always related to arthritis?
No. Arthritis is only one possible explanation for chronic discomfort. Other contributing factors may include connective tissue restriction, repetitive strain, nervous system sensitization, posture related stress, reduced mobility, or muscle imbalance. Some people experience persistent pain despite minimal joint degeneration on imaging scans.
How does hydration influence connective tissue mobility?
Fascia contains water rich material that supports smooth tissue glide between muscles and surrounding structures. Inadequate hydration may reduce tissue elasticity and increase feelings of stiffness. While hydration alone does not cure pain conditions, maintaining proper fluid intake supports overall tissue function and recovery.
Can fascia tightness and pain spread to different body areas?
Yes. Fascial tissue forms continuous chains throughout the body, meaning restriction in one region may influence movement elsewhere. Tight calves, for example, may alter knee or hip mechanics. This interconnected nature sometimes explains why chronic discomfort shifts locations or appears unrelated to the original tension source.
Why do long periods of sitting increase body stiffness?
Movement helps connective tissue remain adaptable and flexible. Sitting for extended periods limits movement variation and may increase tissue compression around hips, spine, and shoulders. Over time, reduced mobility can contribute to stiffness, decreased flexibility, and altered movement mechanics.
Is stretching enough to improve connective tissue health?
Stretching may help temporarily improve mobility, but long term tissue health usually requires varied movement, strength training, adequate sleep, hydration, stress management, and recovery habits. Experts increasingly recommend combining flexibility work with regular physical activity and posture variation for better overall results.