Joint pain after 40 often raises one big question: is it just wear and tear, or something more serious? Many people search for answers around rheumatoid arthritis vs osteoarthritis because both conditions can look similar at first. The truth is, they are very different in cause, progression, and treatment.
This guide breaks down RA vs OA in a clear and practical way. You will learn how to spot the differences early, understand the types of arthritis, and decide when to seek help. The goal is simple: help you protect your joints and avoid long-term damage.
Understanding the Basics of Arthritis
Arthritis is not a single disease. It is a broad term that covers over 100 joint-related conditions. The two most common types are rheumatoid arthritis and osteoarthritis. These two conditions account for the majority of arthritis cases worldwide.
Osteoarthritis is the most common form. It usually develops with age and involves the gradual breakdown of cartilage. Rheumatoid arthritis, on the other hand, is an autoimmune condition. It occurs when the immune system mistakenly attacks the joints.
When comparing inflammatory vs degenerative arthritis, this distinction matters. Rheumatoid arthritis falls under inflammatory arthritis, while osteoarthritis is considered degenerative arthritis.
Rheumatoid Arthritis vs Osteoarthritis: Core Differences
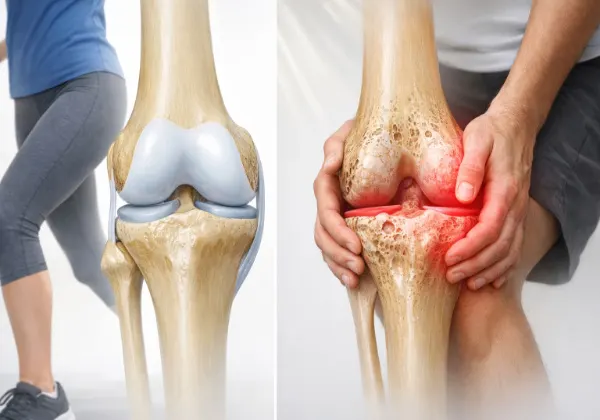
The key to understanding rheumatoid arthritis vs osteoarthritis lies in how each condition starts and progresses.
Rheumatoid arthritis often begins earlier, sometimes between ages 30 and 50. It tends to affect joints symmetrically, meaning both sides of the body show symptoms. For example, both wrists or both knees may hurt at the same time.
Osteoarthritis usually appears later, often after age 45 or 50. It affects joints that bear weight or experience repeated use, such as knees, hips, and hands. Symptoms may start on one side and progress slowly.
Pain patterns also differ. Rheumatoid arthritis causes stiffness that lasts longer than 30 minutes in the morning. Osteoarthritis stiffness usually improves within a few minutes after movement.
Swelling in RA feels soft and warm due to inflammation. In OA, swelling feels harder and relates to bone changes rather than inflammation.
Causes and Risk Factors
Understanding causes helps clarify arthritis differences.
Rheumatoid arthritis develops when the immune system attacks healthy joint tissue. Experts believe genetics and environmental triggers both play a role. Smoking, infections, and hormonal changes may increase risk.
Osteoarthritis develops due to mechanical stress over time. Cartilage wears down, bones rub together, and joint function declines. Risk factors include aging, obesity, joint injuries, and repetitive motion.
This contrast highlights inflammatory vs degenerative arthritis clearly. One stems from immune dysfunction, while the other results from physical wear.
Symptoms Comparison: RA vs OA
Symptoms can overlap, but certain patterns help distinguish RA vs OA.
Rheumatoid arthritis often causes fatigue, low-grade fever, and general weakness. These symptoms occur because the immune system remains active. Joint pain usually comes with redness and warmth.
Osteoarthritis stays localized. It rarely causes whole-body symptoms. Pain worsens with activity and improves with rest.
Joint stiffness behaves differently too. In RA, stiffness lasts longer and feels more severe after inactivity. In OA, stiffness appears briefly and improves quickly with movement.
Finger joints also provide clues. Rheumatoid arthritis affects the middle joints and knuckles. Osteoarthritis commonly affects the end joints, leading to visible bony enlargements.
How Doctors Diagnose Arthritis Differences
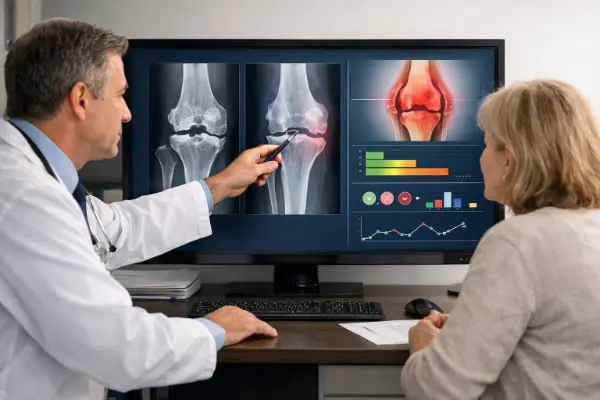
Doctors use a mix of physical exams, imaging, and lab tests to confirm rheumatoid arthritis vs osteoarthritis.
Blood tests play a key role in diagnosing RA. Markers such as rheumatoid factor and anti-CCP antibodies help confirm the condition. Elevated inflammatory markers like ESR and CRP also support diagnosis.
Osteoarthritis does not show up in blood tests. Doctors rely on X-rays to detect cartilage loss, bone spurs, and joint narrowing.
In some cases, MRI scans provide a clearer picture, especially in early RA. Early diagnosis matters because rheumatoid arthritis can damage joints quickly if untreated.
Progression and Long-Term Impact
Rheumatoid arthritis can progress rapidly without treatment. It may lead to joint deformity, reduced mobility, and complications affecting the heart and lungs. Early treatment helps control inflammation and prevent damage.
Osteoarthritis progresses slowly. It mainly affects joint function over time. Pain and stiffness increase gradually, but it rarely causes systemic complications.
This difference makes early detection critical when comparing rheumatoid arthritis vs osteoarthritis. RA requires aggressive early treatment, while OA focuses on long-term joint care.
Treatment Approaches for RA vs OA
Treatment strategies differ significantly due to the nature of each condition.
Rheumatoid arthritis treatment aims to control the immune system. Doctors prescribe disease-modifying antirheumatic drugs, often called DMARDs, to slow progression. Biologic medications may also help reduce inflammation.
Osteoarthritis treatment focuses on pain relief and improving joint function. Doctors recommend lifestyle changes such as weight management, physical therapy, and low-impact exercise. Pain relievers and anti-inflammatory medications help manage symptoms.
If you’re focusing more on managing osteoarthritis symptoms naturally, you may also find this detailed guide helpful: Best Natural Remedies for Osteoarthritis Pain 2026 | Doctor Reviewed Relief Guide.
In both cases, early action improves outcomes. Ignoring symptoms can lead to irreversible joint damage.
Lifestyle Changes That Make a Difference

Lifestyle plays a major role in managing both types of arthritis.
Regular exercise strengthens muscles and supports joint stability. Activities like walking, swimming, and yoga work well for both RA and OA.
Maintaining a healthy weight reduces stress on joints, especially in osteoarthritis. Even a small weight loss can significantly reduce knee pain.
Diet also matters. Anti-inflammatory foods such as fruits, vegetables, whole grains, and omega-3 fatty acids may help manage rheumatoid arthritis symptoms.
Rest and stress management support overall health. Chronic stress can worsen inflammation, especially in autoimmune conditions.
When to See a Doctor
Many people delay medical care, assuming joint pain is just part of aging. That approach can backfire, especially with rheumatoid arthritis.
You should see a doctor if joint pain lasts more than a few weeks, if stiffness persists for more than 30 minutes in the morning, or if swelling appears in multiple joints.
Early diagnosis helps distinguish rheumatoid arthritis vs osteoarthritis and ensures proper treatment. Waiting too long may lead to permanent joint damage in RA cases.
Common Myths About Arthritis
Misunderstandings often confuse people trying to compare RA vs OA.
One common myth says arthritis only affects older adults. While osteoarthritis usually appears with age, rheumatoid arthritis can start much earlier.
Another myth suggests that joint pain always comes from wear and tear. In reality, inflammatory arthritis can cause pain without physical damage in the early stages.
Some people believe exercise worsens arthritis. In truth, proper movement improves joint health and reduces stiffness.
Clearing these myths helps people take symptoms seriously and seek timely care.
Frequently Asked Questions
What is the main difference between rheumatoid arthritis vs osteoarthritis?
The main difference between rheumatoid arthritis vs osteoarthritis is their cause. Rheumatoid arthritis is an autoimmune condition where the immune system attacks the joints, while osteoarthritis is a degenerative condition caused by wear and tear of cartilage over time. RA often affects joints symmetrically and causes inflammation, while OA usually develops slowly in weight-bearing joints.
How can I tell if I have rheumatoid arthritis vs osteoarthritis after 40?
To identify rheumatoid arthritis vs osteoarthritis after 40, look at your symptoms. Rheumatoid arthritis often causes prolonged morning stiffness, swelling in multiple joints, and fatigue. Osteoarthritis usually causes joint pain that worsens with activity and improves with rest, with shorter periods of stiffness.
Is rheumatoid arthritis more serious than osteoarthritis?
When comparing rheumatoid arthritis vs osteoarthritis, rheumatoid arthritis is generally considered more serious because it is a systemic autoimmune disease that can affect organs and cause joint damage quickly. Osteoarthritis progresses more slowly and mainly affects joint function without systemic complications.
Can rheumatoid arthritis be mistaken for osteoarthritis?
Yes, rheumatoid arthritis vs osteoarthritis can sometimes be confused in early stages because both cause joint pain and stiffness. However, blood tests, imaging, and symptom patterns help doctors distinguish between inflammatory arthritis and degenerative arthritis accurately.
What treatments work best for rheumatoid arthritis vs osteoarthritis?
Treatment for rheumatoid arthritis vs osteoarthritis differs significantly. Rheumatoid arthritis requires medications that control the immune system, such as DMARDs, while osteoarthritis treatment focuses on lifestyle changes, exercise, weight management, and pain relief therapies.
Final Thoughts on Rheumatoid Arthritis vs Osteoarthritis
Understanding rheumatoid arthritis vs osteoarthritis can change how you approach joint pain after 40. While both conditions affect joints, they differ in cause, symptoms, and treatment.
Rheumatoid arthritis involves the immune system and requires early medical intervention. Osteoarthritis develops gradually due to wear and tear and responds well to lifestyle changes.
Recognizing arthritis differences early gives you an advantage. It helps you choose the right treatment path and maintain mobility for years to come.
If your joints feel stiff, swollen, or painful, do not ignore the signs. A simple evaluation can provide clarity and prevent long-term complications.
Sources
Centers for Disease Control and Prevention Arthritis Overview
National Institute of Arthritis and Musculoskeletal and Skin Diseases Rheumatoid Arthritis
National Institute of Arthritis and Musculoskeletal and Skin Diseases Osteoarthritis