If your joints could talk, they would probably complain about two things the most: wear and tear or an overactive immune system. That simple contrast sits at the heart of osteoarthritis vs rheumatoid arthritis, one of the most searched and misunderstood comparisons in joint health.
Many people think arthritis is just “joint pain.” That assumption leads to confusion, delayed treatment, and sometimes worse outcomes. In reality, osteoarthritis and rheumatoid arthritis are very different conditions. They have different causes, symptoms, progression patterns, and treatments.
This guide breaks down osteoarthritis vs rheumatoid arthritis in a clear, human way. You will understand what sets them apart, how to recognize early signs, and why getting the right diagnosis matters.
What Is Osteoarthritis?
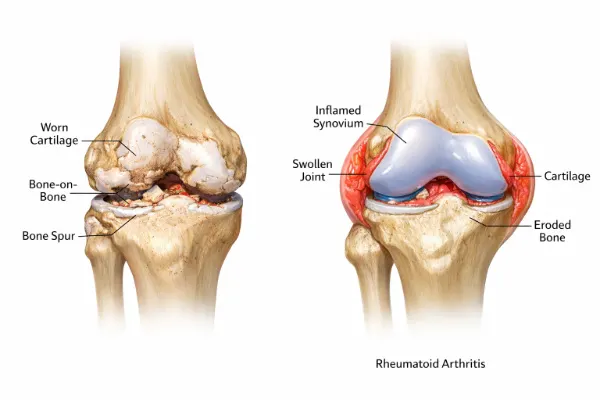
Osteoarthritis is the most common type of arthritis worldwide. Doctors often call it a degenerative joint disease because it develops when cartilage gradually wears down over time.
Cartilage acts like a cushion between bones. When it thins or breaks down, bones rub against each other. That friction causes pain, stiffness, and reduced movement.
Osteoarthritis usually affects weight-bearing joints such as knees, hips, and spine. It can also affect hands, especially in older adults.
Age plays a major role. The risk increases as people grow older. However, osteoarthritis is not just about aging. Injuries, obesity, and repetitive stress also contribute.
In the osteoarthritis vs rheumatoid arthritis debate, osteoarthritis represents mechanical damage rather than an immune system problem.
What Is Rheumatoid Arthritis?
Rheumatoid arthritis is an autoimmune disease. This means the immune system mistakenly attacks healthy joint tissues.
Instead of cartilage wearing out, the immune system targets the synovium, which is the lining of the joints. This causes inflammation, swelling, and eventually joint damage.
Rheumatoid arthritis often affects smaller joints first, such as fingers and wrists. It typically appears symmetrically, meaning both sides of the body show similar symptoms.
Unlike osteoarthritis, rheumatoid arthritis can affect more than just joints. It may impact the heart, lungs, and eyes.
In the context of osteoarthritis vs rheumatoid arthritis, this condition represents a systemic inflammatory disease rather than simple wear and tear.
Osteoarthritis vs Rheumatoid Arthritis: Core Differences
Understanding osteoarthritis vs rheumatoid arthritis becomes easier when you compare their fundamental nature.
Osteoarthritis develops slowly due to physical stress on joints. Rheumatoid arthritis develops due to immune system dysfunction.
Osteoarthritis pain often worsens with activity and improves with rest. Rheumatoid arthritis pain tends to feel worse after rest, especially in the morning.
Osteoarthritis usually affects one side more than the other. Rheumatoid arthritis often affects both sides equally.
Osteoarthritis does not involve widespread inflammation. Rheumatoid arthritis involves chronic inflammation that can damage multiple organs.
These distinctions help doctors diagnose the right condition and guide treatment effectively.
Causes and Risk Factors

When comparing osteoarthritis vs rheumatoid arthritis, the causes differ significantly.
Osteoarthritis develops from long-term joint use. Repetitive movements, injuries, and excess weight increase stress on joints. Genetics may also play a role.
Rheumatoid arthritis has a more complex origin. Genetics, environmental triggers, and immune system abnormalities all contribute. Smoking has strong links with rheumatoid arthritis development.
Hormones may also influence rheumatoid arthritis. Women experience it more often than men, especially during middle age.
Both conditions share some overlapping risk factors, such as age and genetics, but their root causes remain distinct.
Symptoms You Should Not Ignore
Symptoms provide one of the clearest ways to distinguish osteoarthritis vs rheumatoid arthritis.
Osteoarthritis symptoms often include joint pain during movement, stiffness after inactivity, and a grinding sensation. Swelling may occur, but it usually stays mild.
Rheumatoid arthritis symptoms go beyond joint pain. They include prolonged morning stiffness, fatigue, fever, and noticeable swelling. Joints may feel warm and tender.
In osteoarthritis, stiffness usually lasts less than 30 minutes in the morning. In rheumatoid arthritis, stiffness can last more than an hour.
Fatigue is another key difference. People with rheumatoid arthritis often feel unusually tired due to ongoing inflammation.
Recognizing these patterns early helps prevent long-term damage.
How Doctors Diagnose These Conditions
Doctors rely on a mix of clinical evaluation, imaging, and lab tests to distinguish osteoarthritis vs rheumatoid arthritis.
For osteoarthritis, doctors often use X-rays to detect cartilage loss, bone spurs, and joint narrowing.
For rheumatoid arthritis, blood tests play a major role. Doctors look for markers such as rheumatoid factor and anti-CCP antibodies. They also check inflammation levels using ESR and CRP tests.
Imaging helps in both conditions, but lab tests become crucial for diagnosing rheumatoid arthritis.
Early diagnosis matters. Rheumatoid arthritis can cause irreversible damage if treatment starts late.
Disease Progression: What to Expect
The progression pattern highlights another major difference in osteoarthritis vs rheumatoid arthritis.
Osteoarthritis usually progresses slowly over many years. Symptoms may worsen gradually but often remain manageable with lifestyle changes.
Rheumatoid arthritis can progress more aggressively. Without treatment, it may lead to joint deformity and disability within a few years.
Flare-ups define rheumatoid arthritis. Symptoms may worsen suddenly and then improve with treatment.
Osteoarthritis does not usually have flare-ups in the same way. Pain tends to follow activity levels.
Understanding progression helps patients set realistic expectations and manage their condition better.
Treatment Approaches
Treatment strategies differ significantly when comparing osteoarthritis vs rheumatoid arthritis.
For osteoarthritis, treatment focuses on pain relief and joint preservation. Doctors often recommend exercise, weight management, physical therapy, and over-the-counter pain relievers.
In advanced cases, joint replacement surgery may become necessary.
Rheumatoid arthritis requires a more aggressive approach. Doctors use disease-modifying antirheumatic drugs (DMARDs) to slow disease progression. Biologic therapies target specific parts of the immune system.
Pain management remains important in both conditions, but rheumatoid arthritis treatment aims to control the immune response itself.
If you are looking for a joint-friendly workout, this detailed guide on Swimming for Back and Joint Pain: Proven Relief with Low-Impact Exercise (2026 Guide) explains how water-based exercise can reduce pressure on joints while improving mobility.
Early treatment improves outcomes significantly, especially for rheumatoid arthritis.
Lifestyle Changes That Help
Lifestyle plays a key role in managing both conditions, though the strategies differ slightly in osteoarthritis vs rheumatoid arthritis.
For osteoarthritis, maintaining a healthy weight reduces stress on joints. Regular low-impact exercise such as walking or swimming improves flexibility and strength.
For rheumatoid arthritis, managing inflammation becomes the priority. A balanced diet rich in omega-3 fatty acids may help reduce inflammation. Stress management also plays a role.
Sleep matters more than most people realize. Poor sleep can worsen pain perception in both conditions.
Consistency beats intensity. Small daily habits often produce better results than extreme short-term efforts.
Can You Have Both Conditions?
Yes, some people experience both osteoarthritis and rheumatoid arthritis. This situation can complicate diagnosis and treatment.
Doctors must carefully evaluate symptoms and test results to identify each condition accurately.
Managing both requires a tailored approach. Treatment plans often combine strategies used for each condition.
This overlap makes it even more important to understand osteoarthritis vs rheumatoid arthritis clearly.
Common Myths and Misconceptions
Many myths surround osteoarthritis vs rheumatoid arthritis, and they often delay proper care.
Some people believe osteoarthritis is just a normal part of aging. While aging increases risk, severe joint pain is not something you should ignore.
Another myth suggests rheumatoid arthritis only affects older adults. In reality, it can develop at any age, even in young adults.
People also assume all arthritis types share the same treatment. That assumption leads to ineffective management and worsening symptoms.
Education plays a crucial role in breaking these misconceptions.
When to See a Doctor
You should not ignore persistent joint pain, stiffness, or swelling.
Seek medical advice if symptoms last more than a few weeks, worsen over time, or affect daily activities.
Early diagnosis improves outcomes in both conditions, especially rheumatoid arthritis.
Delaying treatment can lead to irreversible joint damage, which becomes much harder to manage later.
Frequently Asked Questions
What is the main difference between osteoarthritis vs rheumatoid arthritis?
The main difference between osteoarthritis vs rheumatoid arthritis is their cause. Osteoarthritis develops due to wear and tear of joint cartilage over time, while rheumatoid arthritis is an autoimmune disease where the immune system attacks the joints. This leads to different symptoms, progression, and treatment approaches.
Which is more painful: osteoarthritis vs rheumatoid arthritis?
Both conditions can cause significant pain, but in osteoarthritis vs rheumatoid arthritis, rheumatoid arthritis often causes more intense and persistent pain due to inflammation. It can also affect multiple joints at once and cause fatigue, making it feel more severe for many people.
How can I tell if I have osteoarthritis vs rheumatoid arthritis?
You can often tell the difference between osteoarthritis vs rheumatoid arthritis by symptoms. Osteoarthritis pain worsens with activity and improves with rest, while rheumatoid arthritis causes prolonged morning stiffness, swelling, and fatigue. A doctor will confirm the diagnosis using blood tests and imaging.
Can osteoarthritis turn into rheumatoid arthritis?
No, osteoarthritis cannot turn into rheumatoid arthritis. In osteoarthritis vs rheumatoid arthritis, they are completely different conditions with different causes. However, a person can have both conditions at the same time, which may complicate diagnosis and treatment.
What is the best treatment for osteoarthritis vs rheumatoid arthritis?
Treatment differs in osteoarthritis vs rheumatoid arthritis. Osteoarthritis treatment focuses on lifestyle changes, exercise, and pain relief, while rheumatoid arthritis requires medications like DMARDs to control the immune system. Early diagnosis is important in both cases for better outcomes.
Final Thoughts
The comparison of osteoarthritis vs rheumatoid arthritis reveals more than just two types of arthritis. It highlights how different the human body can respond to damage and disease.
Osteoarthritis reflects physical wear and tear. Rheumatoid arthritis reflects an immune system gone off track.
Both conditions require attention, but they demand different approaches. Recognizing the differences empowers you to seek the right treatment and improve your quality of life.
If your joints are sending warning signals, listen carefully. They rarely complain without a reason.
Sources
National Institute of Arthritis and Musculoskeletal and Skin Diseases
https://www.niams.nih.gov/health-topics/osteoarthritis
https://www.niams.nih.gov/health-topics/rheumatoid-arthritis
Centers for Disease Control and Prevention
https://www.cdc.gov/arthritis/basics/osteoarthritis.htm
https://www.cdc.gov/arthritis/basics/rheumatoid-arthritis.html
Mayo Clinic
https://www.mayoclinic.org/diseases-conditions/osteoarthritis/symptoms-causes
https://www.mayoclinic.org/diseases-conditions/rheumatoid-arthritis/symptoms-causes
Arthritis Foundation
https://www.arthritis.org/diseases/osteoarthritis
https://www.arthritis.org/diseases/rheumatoid-arthritis
Author Bio
Jennifer Collins is a wellness researcher and natural health writer focused on adults over 40. With 3+ years of experience in digital health content, Jennifer specializes in making science-backed nutrition and lifestyle strategies easy to follow and apply.
Health Disclaimer
This content is for informational purposes only and is not intended to diagnose, treat, or cure any disease. Always consult your healthcare provider before making changes to your diet or health routine. This article may include affiliate links, which come at no extra cost to you.