Waking up with hip pain can ruin a perfectly good night’s sleep. Many adults notice this problem more often after age 50. You lie down comfortably, fall asleep, and then wake up with a sore hip that feels stiff, tender, or even sharp when you move.
If this sounds familiar, you’re not alone. Hip pain when sleeping on side after 50 is a common complaint reported by middle-aged and older adults. Aging changes joints, muscles, and soft tissues. These changes can make side sleeping uncomfortable and sometimes painful.
The good news: in most cases, the cause is manageable. Small adjustments in sleep position, mattress support, and daily habits can make a big difference.
Let’s explore why this pain happens and what you can do to fix it.
Table of Contents
Why Hip Pain at Night Becomes More Common After 50
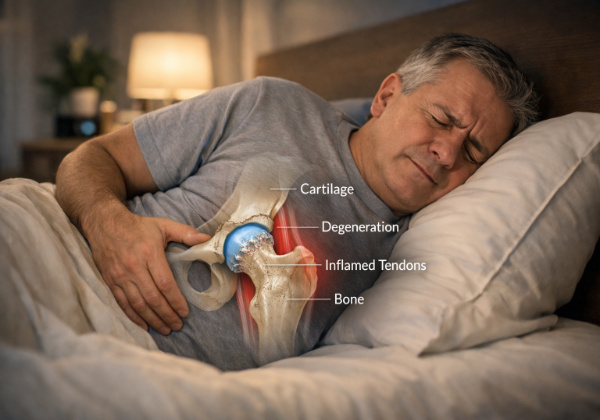
Aging affects the body in predictable ways. Cartilage gradually wears down, muscles lose elasticity, and tendons become more sensitive to pressure.
When you sleep on your side, your hip carries most of your body weight for several hours. This pressure can irritate joints and surrounding tissues.
According to the American Academy of Orthopaedic Surgeons (AAOS), age-related joint changes often increase the risk of hip discomfort, especially during prolonged pressure or repetitive movement.
In simple terms, your hips have worked hard for decades. After 50, they sometimes ask for better support.
Common Causes of Hip Pain When Sleeping on Side After 50
Several conditions can trigger nighttime hip pain. Understanding the cause helps you choose the right solution.
1. Greater Trochanteric Pain Syndrome (Hip Bursitis)
One of the most frequent causes of side-sleeping hip pain is irritation of the trochanteric bursa, a fluid-filled sac that cushions the hip joint.
When this area becomes inflamed, pressure from lying on the hip can trigger pain.
Typical symptoms include:
- Tenderness on the outside of the hip
- Pain when lying on one side
- Discomfort when walking upstairs
- Pain that improves with movement during the day
The Cleveland Clinic notes that bursitis often develops from repetitive stress, aging tissues, or prolonged pressure on the hip.
2. Hip Osteoarthritis
Osteoarthritis becomes more common after age 50. It occurs when the cartilage inside the hip joint gradually breaks down.
When cartilage thins, bones may rub against each other. This friction causes pain, stiffness, and reduced mobility.
Common signs include:
- Deep aching hip pain
- Morning stiffness
- Reduced hip flexibility
- Pain during sleep or after inactivity
According to the Centers for Disease Control and Prevention (CDC), osteoarthritis affects millions of adults and commonly involves weight-bearing joints such as the hips.
Joint wear doesn’t affect only the hips. Similar age-related changes can also impact the knees, especially during movements like squatting or climbing stairs. Our article on Why Does My Knee Hurt When I Bend It After 45? Causes & Fixes explains the most common causes and practical ways to relieve knee pain.
3. Tendon Irritation or Gluteal Tendinopathy
Your hip relies on several tendons, especially the gluteal tendons, to stabilize movement.
Over time, these tendons may weaken or become irritated. Side sleeping places pressure on these tissues, which can trigger pain at night.
Symptoms often include:
- Pain on the outer hip
- Weakness while walking
- Discomfort when standing on one leg
Research published in the British Journal of Sports Medicine shows that gluteal tendinopathy frequently causes lateral hip pain in adults over 40.
4. Poor Mattress Support
Sometimes the problem isn’t your hip. It’s your mattress.
A mattress that is too soft allows your hip to sink too deeply. One that is too firm increases pressure on the joint.
Both situations create uneven spinal alignment. Over several hours, this stress can irritate the hip joint.
Sleep experts often recommend a medium-firm mattress for proper spinal support.
5. Muscle Imbalances and Weak Hip Muscles
Weak hip muscles can also contribute to nighttime pain.
Your glutes and hip stabilizers help distribute pressure across the pelvis. When these muscles weaken with age, the hip joint absorbs more load during sleep.
This imbalance increases pressure on tendons and bursae.
Regular strengthening exercises can reduce this problem significantly.
Symptoms That Often Accompany Nighttime Hip Pain
People experiencing hip pain when sleeping on side after 50 often notice a pattern of symptoms.
Common complaints include:
- Pain when lying directly on the hip
- Pain that improves when switching sides
- Morning stiffness
- Tenderness when pressing the outer hip
- Discomfort during long walks
Pain usually improves during the day because movement increases blood flow and reduces stiffness.
However, persistent pain may signal an underlying joint condition.
How Sleeping Position Affects Hip Pain
Your sleeping position can either reduce or worsen hip discomfort.
Side sleeping concentrates body weight on one hip for several hours. This pressure compresses tissues around the joint.
If the spine or pelvis falls out of alignment, the stress increases.
Small Sleep Adjustments That Help
Try these simple changes:
- Place a pillow between your knees
- Keep your spine aligned while sleeping
- Avoid curling into a tight fetal position
- Alternate sides during the night
These adjustments reduce pressure on the hip and improve alignment.
Simple Solutions for Hip Pain When Sleeping on Side After 50
The right combination of sleep adjustments, exercises, and lifestyle changes can significantly improve symptoms.
Let’s look at practical solutions.
1. Use a Pillow Between Your Knees
This small change often provides immediate relief.
A pillow keeps the hips level and prevents the top leg from pulling the pelvis forward.
Benefits include:
- Reduced hip rotation
- Better spinal alignment
- Less pressure on hip tendons
Orthopedic specialists often recommend this trick for side sleepers with hip discomfort.
2. Improve Mattress and Pillow Support
Your mattress plays a huge role in hip comfort.
Experts recommend:
- Medium-firm mattress support
- A mattress that maintains spinal alignment
- Replacing mattresses older than 7–10 years
Memory foam or hybrid mattresses often provide good pressure relief.
Your pillow also matters. It should keep your neck aligned with your spine.
3. Strengthen Hip and Glute Muscles
Strong hip muscles protect the joint and distribute pressure evenly.
Research published in the Journal of Orthopaedic & Sports Physical Therapy shows that targeted hip strengthening reduces pain in people with hip tendinopathy.
Helpful exercises include:
- Glute bridges
- Clamshells
- Side leg raises
- Step-ups
Even 10–15 minutes of daily exercise can improve hip stability.
4. Stretch Tight Hip Muscles
Tight muscles increase pressure around the hip joint.
Regular stretching helps maintain flexibility and reduces irritation.
Focus on stretching:
- Hip flexors
- Glute muscles
- Hamstrings
- IT band
Gentle stretching before bedtime can relax muscles and improve sleep comfort.
5. Maintain a Healthy Body Weight
Excess body weight increases pressure on hip joints.
According to the CDC, maintaining a healthy weight reduces stress on weight-bearing joints and lowers the risk of osteoarthritis.
Even modest weight loss can significantly reduce hip pain.
6. Use Ice or Anti-Inflammatory Treatments
If inflammation causes the pain, cold therapy can help.
Try applying an ice pack for 15–20 minutes before bedtime.
Doctors may also recommend non-steroidal anti-inflammatory medications (NSAIDs) for short-term relief, though you should always consult a healthcare professional first.
When Hip Pain During Sleep May Signal a Bigger Problem
Most nighttime hip pain improves with simple adjustments.
However, certain symptoms require medical evaluation.
See a doctor if you notice:
- Severe hip pain that wakes you every night
- Difficulty walking
- Pain after a fall or injury
- Hip swelling or redness
- Pain lasting longer than several weeks
Persistent pain may indicate arthritis, tendon tears, or other joint conditions.
Early diagnosis helps prevent worsening symptoms.
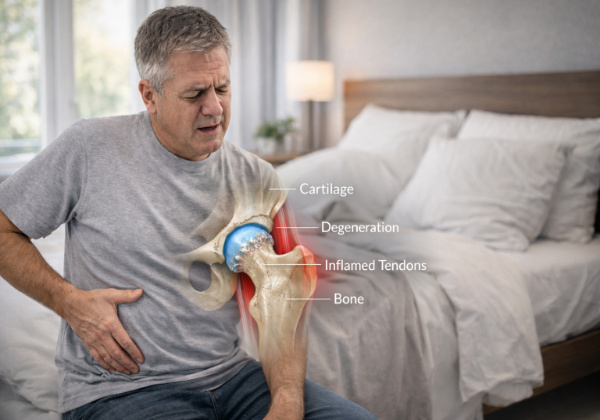
Preventing Hip Pain After 50
Prevention often works better than treatment.
These habits help keep hips healthy as you age:
Stay active
Regular walking, swimming, and strength training support joint health.
Avoid long periods of sitting
Movement keeps joints lubricated.
Stretch daily
Flexibility reduces tension around the hip joint.
Use supportive footwear
Good shoes improve alignment and reduce stress on hips.
Replace worn mattresses
Sleep support matters more than people realize.
Think of hip care like car maintenance. A little attention today prevents bigger repairs later.
A Quick Reality Check: Aging Doesn’t Mean Constant Pain
Many people assume joint pain after 50 is unavoidable. That idea simply isn’t true.
Healthy joints depend on movement, strength, and support.
Most cases of hip pain when sleeping on side after 50 improve with better sleep positioning, stronger muscles, and improved mattress support.
In other words, your hip might not be broken—it may just want a better pillow.
Frequently Asked Questions
Why do I get hip pain when sleeping on my side after 50?
Hip pain when sleeping on side after 50 usually occurs because of age-related joint changes. As cartilage wears down and tendons become less flexible, pressure on the hip during side sleeping can irritate tissues like the bursae or gluteal tendons. Conditions such as hip bursitis, osteoarthritis, and weak hip muscles commonly contribute to this discomfort.
How can I relieve hip pain when sleeping on my side after 50?
To relieve hip pain when sleeping on side after 50, try placing a pillow between your knees to keep your hips aligned. A medium-firm mattress can also reduce pressure on the joint. Gentle hip strengthening exercises, stretching, and maintaining a healthy body weight may also improve nighttime comfort.
Is hip pain at night a sign of arthritis after 50?
Hip pain when sleeping on side after 50 can sometimes be linked to osteoarthritis. This condition develops when cartilage in the hip joint gradually wears down. However, nighttime hip pain can also result from bursitis, tendon irritation, or poor sleeping posture. A doctor can confirm the exact cause through examination or imaging.
Should I stop sleeping on my side if my hip hurts?
You don’t always need to stop side sleeping completely. If you experience hip pain when sleeping on side after 50, try switching sides during the night or using a pillow between your knees to reduce pressure. Some people also find relief by sleeping on their back occasionally to give the hip joint a break.
When should I see a doctor for hip pain during sleep?
If hip pain when sleeping on side after 50 continues for several weeks, worsens over time, or interferes with daily activities, it’s best to consult a healthcare professional. Seek medical attention sooner if the pain follows a fall, causes difficulty walking, or comes with swelling or redness around the hip.
Final Thoughts
Nighttime hip pain can disrupt sleep and affect daily comfort. Fortunately, most cases have clear and manageable causes.
Common triggers include bursitis, tendon irritation, osteoarthritis, and poor sleep support. These conditions often become more noticeable after age 50 because joints and soft tissues naturally change over time.
The good news: simple solutions often work.
Small adjustments—like using a pillow between your knees, strengthening hip muscles, improving mattress support, and maintaining an active lifestyle—can dramatically reduce discomfort.
If pain continues or worsens, a healthcare professional can identify the underlying cause and recommend targeted treatment.
A comfortable night’s sleep shouldn’t feel like a luxury. With the right habits and support, your hips can stay happy well beyond 50
Sources
- American Academy of Orthopaedic Surgeons – Hip Bursitis
- Cleveland Clinic – Trochanteric Bursitis
- Centers for Disease Control and Prevention – Osteoarthritis
- British Journal of Sports Medicine – Gluteal Tendinopathy Research
- Journal of Orthopaedic & Sports Physical Therapy – Hip Tendinopathy Treatment
Author Bio
Jennifer Collins is a wellness researcher and natural health writer focused on adults over 40. With 3+ years of experience in digital health content, Jennifer specializes in making science-backed nutrition and lifestyle strategies easy to follow and apply.
Health Disclaimer
This content is for informational purposes only and is not intended to diagnose, treat, or cure any disease. Always consult your healthcare provider before making changes to your diet or health routine. This article may include affiliate links, which come at no extra cost to you.