Reactive arthritis does not knock before it enters your life. One day you feel fine, and the next day your joints begin to ache, swell, and resist movement. This condition can confuse many people because it often shows up after an infection somewhere else in the body. If you want to understand reactive arthritis symptoms joints in a clear and practical way, you are in the right place.
This guide explains what happens inside your body, why your joints react the way they do, and what symptoms you should never ignore. You will also learn how to recognize early warning signs and what steps you can take to manage the condition effectively.
What Is Reactive Arthritis?
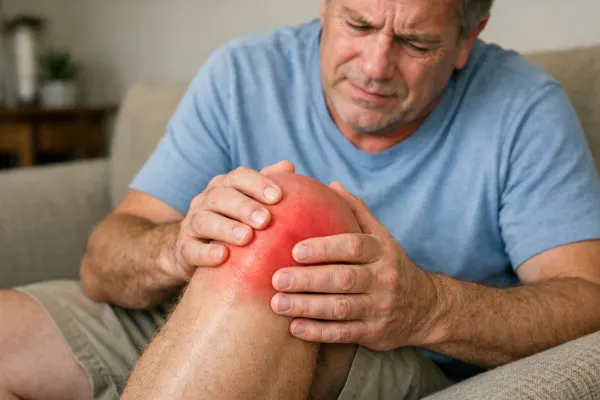
Reactive arthritis is an inflammatory condition that develops after an infection. Most often, it follows infections in the digestive system or urinary tract. Common triggers include bacteria such as Salmonella, Shigella, Campylobacter, and Chlamydia.
The immune system reacts to the infection, but instead of stopping at the source, it mistakenly targets the joints. This reaction leads to inflammation, pain, and swelling. That is why doctors call it “reactive” arthritis. The joints react to something that happened elsewhere.
Many people think arthritis only affects older adults. That is not true here. Reactive arthritis often affects younger adults, especially those between 20 and 40 years old.
Why Joint Symptoms Matter
Joint symptoms often provide the first clear signal that something is wrong. You might brush off mild pain at first, but reactive arthritis tends to progress quickly if ignored.
When we talk about reactive arthritis symptoms joints, we focus on how inflammation shows up in different parts of the body. These symptoms can vary in intensity, but they usually follow a recognizable pattern.
Understanding these signs early can help you seek treatment before the condition worsens.
If you are unsure whether your symptoms match this condition or something more complex, this detailed guide on Lupus Joint Pain vs Arthritis: Key Differences, Symptoms & Diagnosis Guide can help you understand the key distinctions.
Early Joint Symptoms You Should Notice
Reactive arthritis often starts subtly. The first signs might feel like normal fatigue or minor discomfort.
Joint pain usually appears within one to four weeks after the triggering infection. The pain does not always affect both sides of the body equally. Instead, it often targets one side more than the other.
You may feel stiffness when you wake up. This stiffness can last for several minutes or even hours. It tends to improve slightly with movement, but it never fully disappears.
Swelling is another early sign. Your joints may look puffy or feel warm to the touch. This happens because inflammation increases blood flow to the affected area.
Many people also report tenderness. Even light pressure on the joint can cause discomfort.
Commonly Affected Joints
Reactive arthritis does not attack all joints equally. It prefers certain areas of the body.
The knees often take the biggest hit. You may notice difficulty bending or straightening your leg. Walking up stairs can suddenly feel like a workout you never signed up for.
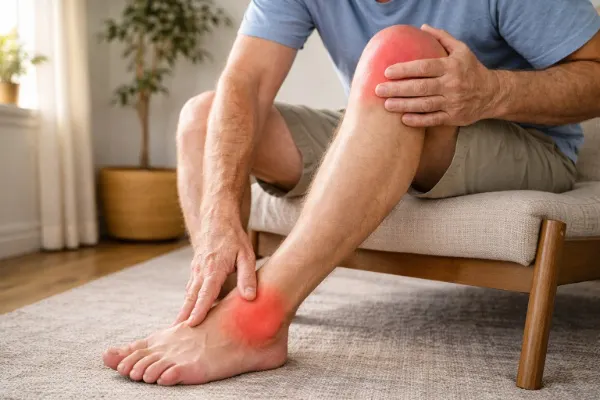
Ankles also become painful and swollen. This can affect your balance and make simple activities like standing or walking uncomfortable.
The feet can show symptoms as well. Pain in the heels is common due to inflammation where tendons attach to the bone. This condition is called enthesitis, and it plays a major role in reactive arthritis symptoms joints.
Some people experience pain in the lower back or buttocks. This occurs when inflammation affects the sacroiliac joints. The discomfort may worsen at night or after long periods of rest.
The Pattern of Joint Pain
One unique feature of reactive arthritis is how it spreads. The condition often affects a few joints rather than many. Doctors call this oligoarthritis.
The pain tends to move from one joint to another over time. You might feel discomfort in your knee today and in your ankle next week. This shifting pattern can confuse people and delay diagnosis.
The symptoms also appear asymmetrical. For example, your right knee might hurt while your left knee feels normal.
This uneven distribution helps doctors distinguish reactive arthritis from other types of arthritis.
Swelling and Warmth in Joints
Inflammation causes visible swelling. The affected joint may appear larger than usual. It might feel warm when you touch it.
This warmth occurs because your immune system sends extra blood and immune cells to the area. While this response aims to protect the body, it ends up causing pain and stiffness.
In severe cases, swelling can limit movement significantly. You may struggle to perform daily tasks like walking, bending, or even holding objects.
Stiffness and Reduced Mobility
Stiffness can feel worse than pain for many people. It restricts your ability to move freely and comfortably.
Morning stiffness is a common complaint. You may feel like your joints need time to “wake up” before you can function normally.
Sitting for long periods can also make stiffness worse. When you stand up, your joints may feel locked or tight.
Regular movement helps reduce stiffness, but it does not eliminate it completely. This ongoing limitation can affect your quality of life if not managed properly.
Tendon and Ligament Pain
Reactive arthritis does not limit itself to joints. It also affects the areas where tendons and ligaments attach to bones.
Heel pain stands out as one of the most common symptoms. You may feel sharp discomfort when you take your first steps in the morning.
Pain can also develop around the Achilles tendon. This makes walking or running difficult.
These symptoms highlight why reactive arthritis symptoms joints often involve surrounding tissues as well.
Joint Symptoms and Fatigue
Inflammation does more than cause pain. It also drains your energy.
Many people with reactive arthritis feel tired even after getting enough sleep. This fatigue comes from the body’s ongoing immune response.
Joint pain and fatigue often go hand in hand. When your joints hurt, you move less. Reduced activity can make you feel even more sluggish.
This cycle can impact both physical and mental health.
When Symptoms Become Severe

In some cases, reactive arthritis becomes more intense. The pain can turn sharp and persistent.
Swelling may increase to the point where joints look visibly enlarged. Movement becomes limited, and daily activities become challenging.
If left untreated, chronic inflammation can lead to long-term joint damage. This makes early recognition of reactive arthritis symptoms joints extremely important.
How Long Do Joint Symptoms Last?
Reactive arthritis often lasts a few months, but the duration varies from person to person.
Some people recover within three to six months. Others may experience symptoms for a year or longer.
In certain cases, the condition becomes chronic. This means symptoms continue or return over time.
The good news is that many people improve with proper treatment and lifestyle adjustments.
What Triggers the Joint Reaction?
The root cause lies in the immune system. After an infection, the body tries to eliminate harmful bacteria.
However, the immune response does not always stop when it should. It continues to attack tissues that resemble the original infection.
Genetics also play a role. People with the HLA-B27 gene have a higher risk of developing reactive arthritis.
This combination of infection and genetic predisposition explains why some people develop the condition while others do not.
Diagnosing Reactive Arthritis
Doctors rely on a combination of symptoms, medical history, and tests.
They often ask about recent infections. If you had diarrhea or a urinary infection before joint pain started, it provides a strong clue.
Blood tests can detect inflammation markers. Imaging tests like X-rays or MRI scans help assess joint damage.
There is no single test that confirms reactive arthritis. Instead, doctors piece together the evidence based on your symptoms.
Treatment Options for Joint Symptoms
Treatment focuses on reducing inflammation and relieving pain.
Nonsteroidal anti-inflammatory drugs, also known as NSAIDs, often serve as the first line of treatment. These medications help control swelling and discomfort.
In more severe cases, doctors may prescribe corticosteroids. These drugs reduce inflammation quickly but require careful use.
Physical therapy plays a key role in recovery. Regular exercises improve flexibility and strengthen muscles around the joints.
Doctors may also treat the underlying infection if it is still present.
Lifestyle Changes That Help
Small lifestyle changes can make a big difference.
Regular low-impact exercise helps maintain joint mobility. Activities like walking, swimming, or cycling work well.
A balanced diet supports overall health and reduces inflammation. Foods rich in omega-3 fatty acids, such as fish and nuts, can help.
Adequate rest is equally important. Your body needs time to recover from inflammation.
Avoid smoking and limit alcohol intake. These habits can worsen inflammation and slow down recovery.
When to See a Doctor
Do not ignore persistent joint pain, especially if it follows an infection.
Seek medical advice if you notice swelling, stiffness, or difficulty moving your joints. Early treatment can prevent complications and improve outcomes.
If pain spreads or becomes severe, it is a clear sign that you need professional evaluation.
Frequently Asked Questions
What are the most common reactive arthritis symptoms in joints?
Reactive arthritis symptoms joints usually include pain, swelling, stiffness, and warmth in affected areas. These symptoms often appear in the knees, ankles, and feet. Many people also notice morning stiffness and difficulty moving after rest.
How long do reactive arthritis symptoms in joints last?
Reactive arthritis symptoms joints can last from a few weeks to several months. In many cases, symptoms improve within 3 to 6 months, but some people may experience longer or recurring joint issues if inflammation persists.
Which joints are most affected by reactive arthritis symptoms?
Reactive arthritis symptoms joints most commonly affect the knees, ankles, and feet. Heel pain is also very common due to tendon inflammation. In some cases, fingers, toes, and lower back joints may also be involved.
Can reactive arthritis symptoms in joints go away on their own?
Yes, reactive arthritis symptoms joints can go away on their own in mild cases. However, without proper care, symptoms may last longer or return. Early treatment can help reduce inflammation and speed up recovery.
What triggers reactive arthritis symptoms in joints?
Reactive arthritis symptoms joints are usually triggered by a bacterial infection, often in the gut or urinary tract. The immune system reacts to the infection and mistakenly causes inflammation in the joints, leading to pain and swelling.
Final Thoughts
Reactive arthritis may sound complicated, but understanding its joint symptoms gives you a strong advantage. The key lies in recognizing early signs and acting quickly.
Joint pain, swelling, stiffness, and tendon discomfort form the core of reactive arthritis symptoms joints. These symptoms may shift, vary in intensity, and affect different parts of the body.
While the condition can disrupt your daily routine, proper treatment and lifestyle adjustments can help you regain control. Stay aware of your body, listen to its signals, and do not hesitate to seek medical guidance when needed.
Sources
Centers for Disease Control and Prevention
https://www.cdc.gov/arthritis/basics/reactive-arthritis.html
National Institute of Arthritis and Musculoskeletal and Skin Diseases
https://www.niams.nih.gov/health-topics/reactive-arthritis
Mayo Clinic
https://www.mayoclinic.org/diseases-conditions/reactive-arthritis/symptoms-causes/syc-20354838
NHS UK
https://www.nhs.uk/conditions/reactive-arthritis/
Cleveland Clinic
https://my.clevelandclinic.org/health/diseases/12145-reactive-arthritis
Author Bio
Jennifer Collins is a wellness researcher and natural health writer focused on adults over 40. With 3+ years of experience in digital health content, Jennifer specializes in making science-backed nutrition and lifestyle strategies easy to follow and apply.
Health Disclaimer
This content is for informational purposes only and is not intended to diagnose, treat, or cure any disease. Always consult your healthcare provider before making changes to your diet or health routine. This article may include affiliate links, which come at no extra cost to you.

